Step-by-step: How to Automate your Claims Processing
by Martha Ducharme - Nov 10, 2022 10:54:53 AM
Discussion on the analog to digital transformation of claims processing has been ongoing for some time now. The importance of automating aspects of claims are often discussed, but some adjusters and other insurance professionals may still be wondering how it works. If you are looking to better understand how your insurance organization can improve, streamline, and automate claims processing, read on:
Map the Customer Journey
No matter how you choose to automate claims processing, the policyholder’s experience needs to be in the forefront to ensure that changes in process provide benefit(s). Kremer and Peddanagari wrote a piece for Ernst & Young regarding the nuances behind proper claims automation. In it, they discuss the philosophy of right-touch handling which focuses on when and where to insert the human element to maximize customer satisfaction.
While every customer may have differing preferences, claims leadership within an insurance organization should be able to map the average intended experience for their policyholders when dealing with a loss. By mapping the customer journey, multiple tracks may be discovered. Understanding which traits lead down one path of claims handling versus another allows you to better determine which claims are best resolved through automation, and which have more complicated handling processes and need an adjuster’s touch to ensure proper resolution. You cannot know which parts of the claim process will require automation without first understanding how customers interact with your current systems.
Incorporating a Multi-Stage Customer Satisfaction System will develop an understanding of the best fit for automation efforts. Likewise, so can the creation of a business rules engine. This entire process enables the creation of Less-Touch and completely Touchless claims flows maximizing efficiency and increasing the coveted customer satisfaction resulting in lower cost adjusting expenses and higher rates of policyholder retention.
The importance of mapping the claim workflow cannot be overlooked. This process brings valuable insight with a strong visual representation of each step to complete the claim handling process. This is an opportunity to audit the process, remove the excess activity, and effectively make adjustments that benefit the customer and the claims team.
Create Rules
When automating claims, parameters must be set to categorize claims to determine which process should be applied. In the past this was done through analog triage, but the creation of automated parameters, or “rules,” allows your claims systems to identify when a claim needs human touch and when it does not. Of course, this means that you can then automate the sorting for claims for right-touch handling, streamlining claims processing while also maintaining high customer loyalty.
With a customer journey already in place, the burden of creating rules has been reduced dramatically. With the knowledge of the most common customer paths established, a rules engine can be employed to perform a variety of functions that will maintain the best path for customers and the business.
Marcin Nowak at Hyperion dove into the functions and components of rules engines, going as far as listing the myriad of functions that rules engines can streamline. This includes customer segmentation, claims classification, claims settlement, price calculation, and various underwriting functions. Knowing that a rules engine can handle a sizable portion of the claims process makes designing one more worthwhile. It also justifies the next step of automating the claims process: integrating with existing systems.
When creating the rules, there is value in knowing when the usefulness has expired or changed. Adding a feature to collect the rule outcome, for example if a rule is consistently not applied or if a rule ‘fails’ to run, allows an organization to continually adjust for the changing business and customer environment.
Prepare for Integration
Creating a new system for claims processing is important, but it cannot stand on its own. At this point, all carriers have existing claims infrastructures, and any new systems or processes added to increase efficiency must be fully integrated into the existing software infrastructure to maximize efficiency. Failure to do so defeats the purpose of automation itself.
Nina Smith of PropertyCasualty360 said, “Disparate systems often lead to scattered data, causing inefficiencies and missed opportunities for payoffs.” This is the exact opposite outcome desired for automating claims processing. This emphasizes the importance of integration. Keeping claims tools easy and effective in the short term but failing to move towards seamless integration will eventually subvert any efficiencies gained by purchasing the tool in the first place. Likewise, a poor interface can also reduce the effectiveness of your automation efforts.
Consider the Interface
After automating the claims process, and completing the internal integration, there is one more aspect of automation to consider: the end user interface. Claims automation integrated with backend systems is one thing but ensuring the ease-of-use for the end user on the front end has equal importance.
Altexsoft gave an example of this aspect when it came to First Notice of Loss (FNOL) automation, stating that the customer-facing interface was one of the two key components of a successful automation system. While many modern automation systems come with user interfaces out of the box, some carriers rely on legacy systems that offer no customer-facing interfaces. No customer interface means that FNOL, or any other claims processes, involving the policyholder requires a phone call for resolution. Analog bottlenecks like this have no place in the digital era of claims handling and must be worked out before the automation can be considered complete.
Simply put, if the customer does not find the product easy to use the end goal of the automation effort will not be achieved.
In Summary
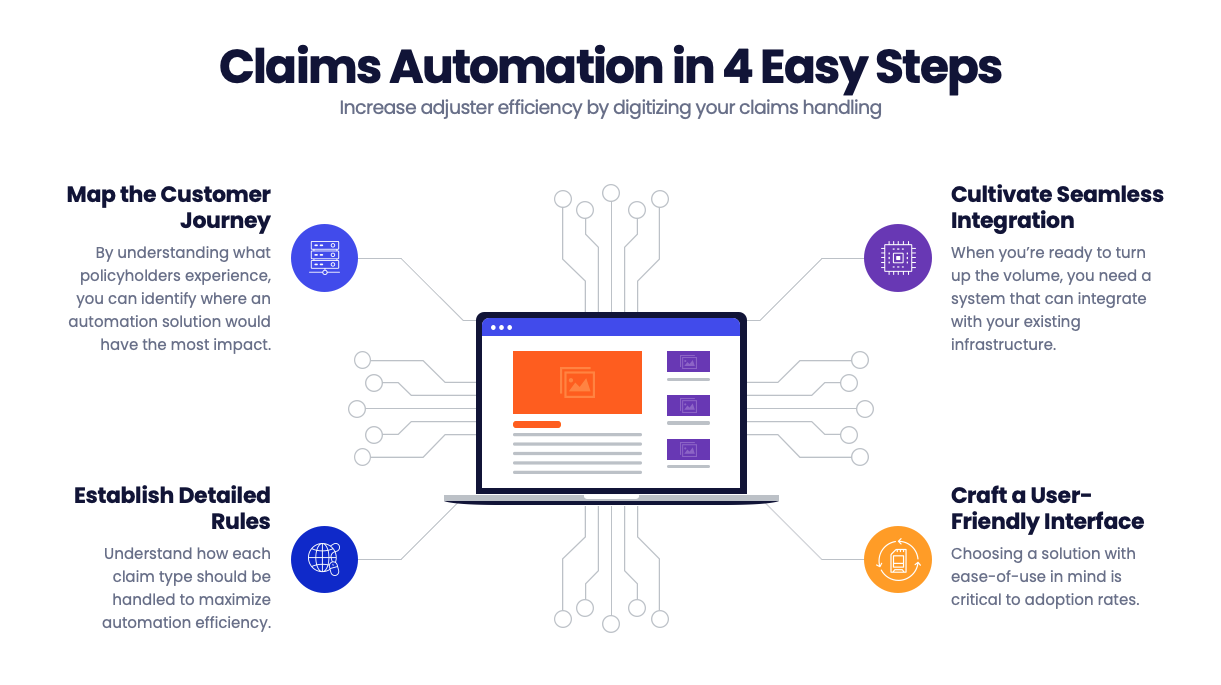
There are four major steps to consider when automating a claims management system (CMS). Each must be considered and accounted for when choosing a provider:
- Map the customer journey
- Establish detailed rules with an audit process
- Seamless integration of the new automation
- User-friendly interface
HOMEE has been on the forefront of the analog to digital transformation of claims processing for some time now, emphasizing adjuster efficiency and high Net Promoter Score (NPS) ratings with its Multi-Stage Customer Satisfaction System. HOMEE’s newest solution, MyCAT Marketplace, keeps the customer in mind while streamlining the catastrophe claim process; it also comes with a multifaceted platform for the adjuster to track catastrophes, connect with restoration professionals based off a series of rules criteria, and is fully integrable with existing claims infrastructure. Click here to sign on today.
ABOUT HOMEE
HOMEE is leading the digitization of property claims. HOMEE’s pioneering technology connects insurers, policyholders, and skilled service providers throughout the lifecycle of a claim. The HOMEE Digital Marketplace & Claims Management platform, in combination with a highly curated network of service providers, is utilized by leading firms in the insurance sector to dramatically improve the claims experience for policyholders. HOMEE is backed by investment from leading insurance companies such as Liberty Mutual, State Farm, The Hartford, Desjardins, and Ferguson Ventures. For additional information on the HOMEE Claims platform visit www.HOMEE.com.




